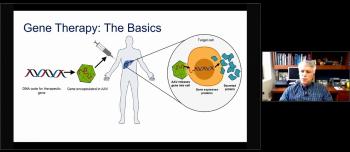
What exactly is meant by individualized therapy? What might be the future treatment and quality-of-life implications for hemophilia patients? Learn more about this state-of-the-art approach to care, and how it could improve the health of a person living with hemophilia.
Transcription of "One Size Does Not Fit All: Individualized Therapy"
KELLEY POLLARD (Moderator): Good evening, and welcome to One Size Does Not Fit All: Individualized Therapy, part of the National Hemophilia Foundation’s Hemophilia Webinar Series. This series is supported by an educational grant from Novo Nordisk. Our presenters this evening are Dr. Steven Pipe and Dr. Margaret Ragni.
Dr. Pipe is a Professor of Pediatrics and Pathology at the University of Michigan in Ann Arbor, and Medical Director of the University’s Pediatric Hemophilia and Coagulation Disorders Program. He is also chair of NHF’s Medical and Scientific Advisory Council.
Dr. Ragni is a Professor of Medicine at the University of Pittsburg and Director of the Hemophilia Center of Western Pennsylvania. She is also a member of NHF’s Medical and Scientific Advisory Council.
Welcome, Dr. Pipe and Dr. Ragni.
So, our program will conclude with a question and answer segment. To ask a question, go to the area in the far lower left of your webinar screen and type your question in the field just to the left of the Send button, which is located in the pod area labeled Chat. Click the Send button when you have finished typing your question. However, please note that your question will be addressed during the question and answer session at the end of the presentation.
There are no handouts for this presentation, however, a recording of this webinar will be available shortly on the National Hemophilia Foundation website, which is www.hemophilia.org.
And now I would like to turn things over to Dr. Pipe.
DR. STEVEN PIPE: Greetings to everybody. I’m glad that you could take the opportunity to participate in this webinar today. I’m going to give you an overview of hemophilia and the state of care today and where there are still some areas for continued improvement. We’ll end with some updates on some of the new products which are beginning to transform care for our patients with hemophilia.
Just as some background, as many of you likely know, hemophilia refers to a deficiency or a dysfunction of clotting factor VIII, or factor IX, otherwise known as hemophilia A or hemophilia B. They’re both clinically indistinguishable. They’re both what we call X-linked disorders, which means males are typically affected, whereas females are carriers, although rarely females can have symptomatic disease.
Clinically the hallmark of bleeding in hemophilia is bleeding into the joints and into the muscles and soft tissues. The severity and the risk of that bleeding, however, is pretty well determined by the residual amount of factor activity that can be measured in the blood. So, patients with severe disease truly have less than 1% residual activity, and often have zero. These are the patients who are at risk for spontaneous as well as traumatic bleeding. At the other extreme, having as little as over 5% makes bleeding into the joints very unusual, and most bleeding is triggered only by trauma. And then in between is moderate where as little as 1% to 5% activity seems for the most part to prevent spontaneous bleeding, but patients can still be at risk for joint bleeds with even relatively minor trauma.
The goal of modern therapy is to completely prevent bleeding. We’re going to show you that that has been achieved generally by maintaining factor levels.
The half-life of the product that’s infused for factor VIII is a little bit shorter, only about eight to twelve hours, whereas for factor IX it’s anywhere from twelve to 24 hours. So, both products require relatively frequent injections. But because of the shorter half-life for factor VIII, factor VIII prophylaxis regimens typically involve at least three infusions per week or every other day, whereas for factor IX most patients are on a twice-weekly.
The history of hemophilia goes back to the 1800s where at least clinical cases can be described. It really wasn’t until blood transfusion technology arrived in the latter half of the 1800s that there were any therapies available. Of course, Queen Victoria and the royalty in Europe made hemophilia somewhat infamous. This was particularly true for Prince Alexei as part of the Russian royal family. You have to fast forward all the way to only about the last five years or so where it was finally determined that within the queen’s family it was hemophilia B as the inherited disorder.
The biggest breakthrough for treatment for hemophilia was in the 1960s with the availability of cryoprecipitate. This was a unique derivative from blood products. This for the first time allowed us to raise levels that could really get on top of bleeding. Then through the ‘70s and ‘80s we were able to purify to high purity the individual factors for factor VIII and factor IX and could really raise plasma levels to whatever was needed.
Another breakthrough was the cloning of the factor VIII and the factor IX genes in the early ‘80s, and that ushered in the recombinant era using cell culture technology for more than twenty years. Now we’ve been able to make recombinant copies of factor VIII and factor IX. Those have taken over as the primary thrust of therapy in the recent decades.
It’s in the last few years that we’ve seen further advances on the recombinant platform with extended half-life technology, which we’re going to talk about today. But I’ll also show you that there are some new paradigm shifts coming: some novel non-factor replacement therapies that are showing promise as well as we have the first real promising results from gene therapy for both factor IX as well as factor VIII.
This slide is just showing some of the waves of paradigm shifts in managing hemophilia. In the olden days it was focused on pre-replacement therapy. That meant supportive care. Patients describe spending much of their time in hospitals or bedridden at home. Patients were destined for recurrent, acute and chronic pain, debilitating joint disease, and there was high mortality.
Once we had the replacement therapy era, initially it was on demand, but it soon became evident that prophylactic therapy could offer the chance to preserve joints well into adulthood. We now have effective bleed treatment and prevention with these therapies. It allowed for home-based care. What has happened in the extended half-life era is we’ve been able to reduce the intensity of that home-based care.
Inhibitor risk has emerged in this era because of the intensity of factor replacement. We’re still dealing with that going forward, but we’ve dramatically reduced the morbidity from joint disease. We really expect the current generation of patients to live normal lives.
The non-replacement therapies are agents that don’t involve replacing factor VIII or factor IX, and have a number of different strategies that target the inhibitors of coagulation. They’re showing great promise to also provide prophylaxis. They will be amenable to home-based care. They’re relatively low intensity. And, more importantly, they’re liberating patients from IV infusions.
Some even greater promise from these products is because they don’t involve exposure to factor VIII or factor IX. They might ameliorate the inhibitor risk in patients.
We’re awaiting this next shift to gene therapy with promise of raising levels well into the mild range and possibly even completely curative. That would be a discussion for another day, but I think that’s the next paradigm shift to come.
This is just showing you the primary outcome data from the definitive clinical trial that showed the benefits of prophylaxis. This was a randomized control trial in toddlers with severe hemophilia A. They were all less than 30 months of age. It was performed in the U.S. They did a randomized comparison to patients who were placed on on-demand therapy where they were just treated when they had breakthrough bleeds versus being on a prophylactic regimen of three or four doses per week.
Highlighted in blue are the most important points. First off, the number of joint bleeds that were experienced in the prophylaxis group. This is the number per year. You can see that the patients on prophylaxis had essentially zero bleeds per year compared to about four for those who were on standard or on-demand therapy. Importantly, because the follow up here was only about five years, it was hard to identify the impact on joints without detailed radiologic studies. So, they used a very sensitive technique using MRI. What they are able to show is that 93% of the patients on prophylaxis had no evidence of joint damage by MRI, whereas about half of the patients with standard therapy had evidence of injury. So, this definitively showed that prophylaxis prevents joint damage and prevents bleeding, and is now the standard of care in most of the developed world.
So, we know that prophylaxis reduces joint bleeds. It reduces joint damage even with sensitive measures by MRI. It’s the standard of care for severe hemophilia, but there are some challenges. We mentioned the frequent injections. It’s invasive. It requires venipuncture. In fact, half of adults still avoid prophylaxis because they’re not keen to do the intensity of treatment and to do the venipunctures. Ports are often required as a form of venous access in children whose peripheral venipunctures are inadequate. Most children, even starting in infants, are receiving at least one infusion per week. So, this is a really significant burden ongoing for a young patient.
I mentioned the goal of prophylaxis has been to maintain factor levels above 1%. This is data that supports that strategy. This is derived from large clinical trial databases where they knew what the individual pharmacokinetics were for the infused factor, and they also knew the number of bleeds that patients had and the timing of those bleeds. What was interesting is they could calculate how many hours a week a patient would spend where their factor level would dip under 1% on these trials. Then they would have a measure of a prediction of how many bleeds they would have over the course of a year by spending that amount of time below 1%. You can see that there is a strong correlation here that as you increase the number of hours per week that you spend less than 1%, the predicted number of bleeds per year goes up substantially. So, this kind of data has continued to support the overall goal of trying to maintain a fracture level of at least 1% to prevent spontaneous bleeding.
If we look at clinics that have been doing prophylaxis in this fashion for many, many years, we still see that there are patients who are still having some evidence of recurrent bleeding and evidence of early joint disease. This is exemplified in this graph here. This comes from the pediatric clinic in Bonn, Germany. They were at the forefront of prophylaxis early on in the developed world. This is what we would call a schematization looking at the long-term trajectory of joint outcomes in patients in their clinic over time. What you should see across the bottom is the advancing age of the patient. These are patients who were followed over 25 to 30 years. Using different scoring tools that assess the status of joint deterioration, they could score the joints of the individuals as evidence of background bleeding that was leading to joint damage. Just using an arbitrary threshold here of a joint score of 2, an indication of a clinically meaningful injury to the joint, you can see throughout early childhood in this gray box patients are really pretty clinically silent. We don’t see any evidence of joint damage. Generally they are having very infrequent bleeding.
But if you look at the trajectory over 25 to 30 years, we can see that there is this pattern of ankles having more advanced damage compared to knees and elbows. If you look at two different types of examinations of the joints—this is a Gilbert scale, which uses a clinical examination versus a Pettersson scale, which is radiological, so a little bit more sensitive—you can see that even out 25 to 30 years patients are just barely showing evidence of joint damage, but if you look at it radiologically there are patients who clearly have evidence of joint damage over time. This tells us that even with really aggressive prophylaxis, some patients are still having some background bleeding that is leading to advancing joint disease.
This is also exemplified in the U.S. population from a recent cohort study done through the Centers for Disease Control. This is the data collected over many years in cooperation with the CDC. They broke up the participants in this study in different birth eras. These are individuals who were born prior to 1958 all the way up to the so-called modern era, which were boys who were born between 1983 and 1992. This age group of patients would have been the patients who should have benefited the most from the application of prophylaxis. They asked the question in this study, “Did we close the gap between patients with severe disease and those with mild disease?” meaning did we make it so that the severes who were placed on prophylaxis looked more like patients with mild disease. The answer from this study is no. If you just look at the bottom just looking at bleeding complications, individuals who reported less than or equal to two joint bleeds in the preceding six months, patients with mild disease in this era, 95% would have said that was true, but only about half of the severes said that was true. For individuals reporting more than or equal to five joint bleeds in the last six months, you can see that’s extremely unlikely in mild disease, but still about a third of the patients in this birth cohort were having that much bleeding. I think by any measure we would say that that’s an unacceptable amount of ongoing bleeding.
So, what’s the challenge in trying to get control of bleeding? The trouble is that it’s not just based on that trough level. That’s one component. But the trough level is going to be determined by the interval of treatment, meaning the closer together you do your dosing, the likelihood that the trough level will be higher. You can also drive those trough levels up by using a lot more factor, but with that comes significant cost. What we’ve been able to do in the last couple of years is work with modified factors that have a longer half-life, and in some cases that’s either been able to stretch out the interval or to raise the trough level in patients.
There are all different kinds of bleeding triggers based on the physical activity of the child or the young man. Whether they have background arthropathy or chronic synovitis, all of these are going to lower the threshold to make bleeding more likely.
I’m going to give you a clinical case that’s sort of adapted from a real case in our clinic. This was a boy with severe hemophilia A, and in infancy and early childhood he was placed on primary prophylaxis. So, he hadn’t had any joint bleeding yet, and he was on a pretty good regimen of 40 units per kilo of recombinant factor VIII every other day. But the family admitted that they had a difficult time being adherent to this regimen. But even so, early on his joint bleeds were pretty infrequent—less than one per year. But once he hit school age he was more active, including some sport participation, and he started to develop a right ankle target joint, so repeated bleeding into the same joint. We know that’s going to ultimately lead to joint damage if we don’t get on top of that.
Unfortunately the family continued to struggle with adherence. They were usually dosing about two to three times per week, but he was still having sporadic bleeding into his right ankle. On physical exam he had all the features of what we would call chronic synovitis.
These were the actual options that we discussed in clinic with the family. We continued to push for the traditional prophylaxis regimen until he’d had full resolution of the target joint bleeding, but we thought that the family would likely continue to struggle with adherence and he wouldn’t be much further ahead. There are techniques, such as surgical or radionuclide synoviorthesis to try to reduce the amount of synovial inflammation, but that involves some sort of a surgical procedure with some adverse event risk. And it wasn’t clear that with the prophylaxis following the procedure that we were going to be able to control his bleeding effectively.
We could have asked him to stop participating in the physical activity that might have been triggering the bleeds, but that really wasn’t a good option in this case. There are options to really figure out his individual pharmacokinetics and use an individualized approach to really make sure that his level was never dropping below 1%. And there have been clinical studies that have supported that approach, however, that would be highly dependent on being strictly adherent to the regimen.
The other consideration was to use an extended half-life factor VIII that would achieve higher trough levels than we were getting with his traditional factor VIII. In fact, that’s what we did. We switched him to an extended half-life factor VIII product. We were now achieving trough levels with every-three-day dosing of 7% or 5% by two different factor VIII measures. We noted that his right ankle target joint bleeding completely ceased, and six months later on physical exam he had no evidence of joint swelling or reduced range of motion, and he was now ready to start to return to regular sports participation.
So, I think this highlights the advantages of the extended half-life products that we have available.
I want to spend a few minutes to show you how this technology has been applied. We have extended half-life proteins. I mentioned the novel non-factor therapies. I think this is really exciting innovation. These are really going to be paradigm shifts going forward. They will allow reduced dosing frequency, better protection from bleeds, I mentioned that there could be some reduced immunogenicity and, in some cases, avoiding intravenous administration and going to a subcutaneous route at least for the novel non-factor therapies.
If you followed some of the presentations in recent years about prolonging the half-life of clotting factors, lots of different techniques are being applied.
You might have heard years ago about a liposome delivery system. In this case the liposomes would be a delivery vehicle to try to extend the lifespan of the factor. That was tried in a clinical trial, but it really didn’t achieve the pharmacokinetic results that were needed, and so nothing was further pursued.
But two other techniques have shown better efficacy in that regard. You can chemically modify the recombinant factor VIII with adding a conjugate called polyethylene glycol. This makes the molecule appear bigger in the body, and it buffers the protein away from the receptors that would clear the factor from circulation and prevent it from being degraded. That extends the half-life.
The other alternative is to take advantage of a natural recycling mechanism at the cellular level. Normally factor VIII or factor IX or other plasma proteins get taken up into the cell and get sent to the so-called garbage cans of the cell, or the lysosomes, where they’re degraded, and that’s how they’re cleared from circulation. But if you add either albumin as a fusion to the factor or a portion of an immunoglobulin antibody called the Fc fragment, this allows those proteins that contain those fusions to interact with something called the neonatal Fc receptor. Once it gets taken up intracellularly, instead of going to the garbage cans of the lysosomal degradation, it gets recycled back to the cell surface and it continues to circulate in the plasma. Both of these latter techniques have shown that they can extend the half-life of the product significantly.
This was best exemplified with the factor IX products. Whether it’s Fc fusion or albumin fusion or pegylation, all of these resulted in anywhere from three- to fivefold longer half-life in circulation for factor IX, and this has dramatically reduced the frequency of infusions for these extended half-life factor IX products. Most patients can be treated on these products once a week, and, in some cases, can stretch out their interval to every two weeks, so a real significant change.
For factor VIII there is an Fc fusion product as well as multiple pegylated products. Only one has been approved so far, but the others are all in late trials and we expect them to ultimately be approved. The liposome one, as I mentioned, was discontinued. These have all shown on average an increase of about one-and-a-half times the standard recombinant factor VIII, so not as significant as for factor IX, but still enough so that patients will probably infuse at least one dose less per week than they were with their previous standard product and, as I showed you before, also can achieve higher trough levels.
Just so you have a few visual pictures to see what this looks like, this is one example of a pegylated factor VIII. This is a schematic showing what factor VIII looks like. What they did is they introduced a single substitution of one of the amino acids in the protein, and that allowed them a place to conjugate the PEG moiety to the molecule. That’s what gives it the properties that we mentioned.
Here is another example. This is what factor IX looks like. Here you can see that they conjugated this PEG group that increases the bulk size of the protein. Uniquely this was conjugated in a specific place called the activation peptide. So, when this factor IX gets activated so that it’s functional, this activation peptide is released, the pegylation portion leaves the molecule and you’re left with just the native activated factor IX protein that looks just like the native molecule.
Here is an example of where they did the conjugations here. This is showing that this activation peptide is excised out leaving the factor IX left behind.
Here is what the albumin fusion protein would look like. Here is the factor IX. But in this case, because albumin is such a large protein fusion, it had to be conjugated at the tail end of the molecule. And because the factor IX gets activated before it’s functional, the albumin group is too big here and it gets in the way, so they uniquely engineered a cleavage sight right here so that when the factor IX gets activated, that albumin portion floats away from the molecule and you’re left with the native factor IX for its function. This was a really innovative strategy to take advantage of the half-life extension, but not interfere with the function of the molecule.
This is what the Fc fusion would look like. This is the factor VIII molecule up here. The Fc portion that comes from immunoglobulin is conjugated to the end of factor VIII. Uniquely for this molecule, this Fc doesn’t seem to get in the way of the functional properties of factor VIII, and so it does not have to be cleaved off the protein for factor VIII to be functional.
This is just showing where the Fc portion is fused directly to the tail end of factor VIII. The business portion of factor VIII where all of its functional capacity is, is in these A domains and in the C domains. Just related to how they did the conjugate here, the Fc does not get in the way and it remains functional.
So, that’s the background biology for these new extended half-life factors. Now we’re going to hear from Dr. Ragni about how the clinical trials have demonstrated the efficacy of the proteins and how they have the hope to continue to transform care for patients.
DR. MARGARET RAGNI: Good evening. I am delighted to be here to talk with Dr. Pipe, who did a great job on the first half of our program. My goal here today will be to review the findings of some of the clinical trials of these extended half-life proteins, and then to talk just a little bit about the experience with patients, including some at my own center, and how one might consider using extended half-life proteins in real life.
On this slide, which is a rather busy slide, I have summarized what we know from clinical trials about both the recombinant factor VIII extended half-life proteins, and we have the Fc, the glycopegylated. These are all pegylated proteins. And then with the recombinant factor IX extended half-life proteins, the Fc IgG that you heard about, the albumin fusion protein anti-glycopegylated protein.
The first thing I want you to know is among the factor VIII proteins, over 570 patients were involved in these studies using a dose between 25 and 50 units per kilogram, which was given once or twice or more a week. In these patients, they had very few bleeds, as you can see here. This is an annualized bleed rate of 3, 1, almost 2. Almost everyone had a good response. There were no inhibitors, but none were expected, because these were previously treated patients. But here is what’s really interesting: they all had between 1.4- and 1.5-fold extended half-life, which is what is so critical to reduce the burden of treatment that Dr. Pipe so clearly talked about. So, instead of having to treat three times a week, one might go down to twice a week and in some cases once a week. And we’ll talk about that in a minute.
With the factor IX proteins, there were fewer patients—about 150—treating between a 40- and 100-unit per kilogram dose every one to two weeks or ten days, and, as you can see, a very low rate of an annualized bleeding event, very high response rates, no inhibitors. Again, none were expected, because these were already treated patients. And here you can see that there was an extension in the half-life between 2.5- and 5-fold allowing them to treat much less frequently than currently done.
So, what were the findings in these clinical trials? In general, for all of these proteins that we just looked at, they were safe, they were well tolerated, they improved the half-life and recovery and delayed the clearance of these proteins. None had any inhibitor development. There were no allergic reactions, no thrombosis and the efficacy was considered comparable to recombinant factor VIII and recombinant factor IX. And the safety was comparable. These were not randomized trials. The results of the half-life proteins were compared to what we know from previous trials of recombinant factor VIII and factor IX.
Here are some images that we can look at. On the left is an extended half-life factor VIII protein. On the right is an extended half-life factor IX protein. In these circumstances I’m using the Fc factor VIII and the Fc factor IX, because these were the first studies that were done. These are what we would just call fall-off curves. What you’re doing on the bottom line of the graph is that’s the time between giving the first dose and watching over the course of a week what one might see. Clearly in the gray here is the standard recombinant factor VIII. The blue is the Fc factor VIII. You can see there is an extension of its half-life such that you can remain above 1% for 1.5-fold longer than you did with the recombinant factor VIII allowing one to the treat SHL as standard half-life 25-25-50 units per kilogram on a three-times-a-week basis, which is what’s currently done with recombinant, whereas the extended half-life could be given twice a week, and the most commonly used regimen was 25 units per kilogram such as on a Monday, and 65 units per kilogram such as on a Thursday for the recombinant factor VIII Fc.
Similarly you see a very similar kind of finding with the red recombinant factor IX Fc compared to the dotted line, which is the standard recombinant factor IX, which extends that half-life and extends the time that you were above 1% presumably preventing bleeds during that time, and that while you took 75 units to 100 units per kilogram twice a week with recombinant factor IX, now you could take a 75- to 100-unit per kilogram dose once a week. A major improvement for many patients even thinking they would consider prophylaxis had they not been on it before, because it was so much easier to do.
This brings us to the next slide, which asks: what are the potential implications of having an extended half-life protein? Some of those include a longer duration that the factor level is above 1% that results in fewer and less-frequent infusions. One could imagine that if a port was needed for frequent infusions and you could get it down to twice a week or even once a week, one could actually avoid a port. The problems there of course are infections, sepsis, emergency room visits, hospital stays, cost and a very poor quality of life. In addition, there might be fewer interruptions from school or work and an improved quality of life.
What about this improved half-life? One of the interesting findings in the clinical trial of the factor VIII Fc protein was that in children especially, and even half the adults, if you gave a single dose of the recombinant factor VIII Fc at a standard dose of 50 units per kilogram every five days, they found that by the time of the next dose, if they just gave it once a week, they had no factor level above 1%. They said, “Boy, that’s unusual. Why would you have no bleeds?” Well, some of our pharmacologic experts had shown us why that is. In fact, this explains why we are able in very young children to give this protein once a week and prevent bleeds even though by the end of the week we may be lower than 1%. So, on the left you’re seeing the standard recombinant factor VIII under the curve. We call it AUC—area under the curve, the time spent greater than 1%, which is that protection from bleeds. But look where that AUC is for the patient who’s getting a recombinant factor VIII Fc. It’s much prolonged. In fact, even though it falls below 1%, there is a much prolonged time period or protection, that is area under the curve that time period greater than 1%.
In fact, if you wanted to compare the standard half-life recombinant factor VIII on the top level here, SHL, with the lower panel, what you see is to achieve that longer half-life, one needs to have a slightly higher peak. So, as you will recall, we had originally said that we would use a 25-25-50 unit per kilogram for recombinant factor VIII, whereas we go as high as 65 units per kilogram for that recombinant factor VIII Fc just to do the comparison.
This brings us to a very interesting question. How does each patient look when we try to do this? Does everyone use the same dose to achieve greater than 1%? Absolutely not. And, by the way, this data is from Spotts, who presented it on standard recombinant factor VIII clotting factor, but it actually applies to all clotting factors. What they did was they showed that you have to individualize the dose. What they did was they did pharmacokinetics in 34 severe hemophilia A patients, and what they showed was that an individual dose to achieve a trough of 1% for each patient—what it was. They then determined what it required to prevent a bleed and what the optimal prophylaxis dose was. And in these 34 patients the median factor VIII required to prevent a joint bleed was 3%—3.43. To prevent other bleeds it was almost the same, 2.87 units per deciliter, and to prevent spontaneous bleeds it was 2.71. But, remember, these are medians. That means the middle of the group.
Please look over here at this graph on the right where it looks at the time of a bleed after infusion. It’s highly variable for all of these patients. What’s critical is to recognize that we really do need to individualize dosing for our patients. How do we do that? That’s what we’re going to talk about in a minute. On this slide I’m just showing you that in his study he found that 76% were bleed-free greater than a level trough of 5%. That means that 24% were not, and 94% were bleed-free when their trough level was greater than 15%, meaning 6% were not. So, a lot of this has to do, as Dr. Pipe mentioned, with your activity level and many other factors that are critical to people’s lives and their individual genotype and phenotype.
That brings us to what I think are some of the critical questions we need to ask. Who should use extended half-life proteins? Some of the questions are: will these delay the onset and reduce the type and frequency of bleeds? What about prophylaxis? Will extended half-life proteins simplify or encourage prophylaxis? And what dose and what trough are critical to accomplish effective prophylaxis? Number three, what about chronic joint disease? Will extended half-life proteins slow the onset of joint disease? Will they reduce the severity of joint disease? Or even prevent joint disease surgery, which is so commonplace in our adults who have bad disease? And what about inhibitor formation? Will extended half-life proteins reduce inhibitor frequency with a titer or shorten immune tolerance?
These are critical questions. I’m going to tell you right here and now, I don’t have all the answers but I would like to show you what we do know and why there is such excitement about these proteins.
Let’s talk about prophylaxis, bleeds and joint disease. In order to demonstrate that these extended half-life proteins reduce the annualized bleed rate, which is ABR, number of infusions or the time of less than 1%, or improve joint preservation, we really need to do prospective data collection. What you need to know is that there is something called [inaudible 41:54], which you’re probably already involved in at your hemophilia center. This is a very critical surveillance network in which data are collected. We collect data on joint health, quality of life, pharmacokinetics and we are even able to do cost-effectiveness analyses once this data is collected. It is critical for all patients to participate to allow us to understand are these helping you? Are these helping most people? Are they only good for a certain group of patients? Of course we suspect they’re good for everyone, but we need some data to show that.
Number two, what about inhibitor formation and tolerance? In order to demonstrate that these extended half-life proteins may reduce the immunogenicity, that is immune reactions to factor VIII, that is inhibitor formation—to improve and shorten immune tolerance we need prospective data collection. At least two studies have actually started to collect preliminary information and are starting to show that there is great hope that these extended half-life proteins can prevent inhibitors and shorten immune tolerance. I’ll be showing you just a little bit of information on that.
In fact, here are those two studies. One is called the INHIBIT study. This is a study in which we are proposing that this recombinant factor VIII Fc will prevent inhibitor formation if it’s given weekly beginning before a bleed in young PUPs, previously untreated patients. This was done in mice. Squeak-squeak. I know you probably say to yourself, “Why is she talking about mice?” Many of the important discoveries and new novel therapeutics we’re using were first tested in mice, including the extended half-life recombinant factor VIII Fc. What they showed in mice was that it reduced inhibitor formation from 80% in nearly all the mice down to about 10%, and it reduced the titer. In our study we’re going to look at the exact same thing in young children.
Number two, the HIRE study, which I am doing along with one of my younger colleagues. We designed it to look at whether or not recombinant VIII Fc might shorten immune tolerance, because if it in fact improves tolerogenicity that reduces the immune response to factor VIII it should shorten immune tolerance. In fact, we’ve done about a half a dozen now, and a number of different centers are looking at this. We’ve been able to shorten immune tolerance into one month. We know this is nine months. We need long-term studies to see if this really is true in all patients or just some patients. But what I’m showing you this information for is to tell you we need to work together, we need to collect data together and we need to do clinical trials together in order to get these answers, which will be so helpful to the hemophilia population.
What I wanted to show you on the next slide was what we have found in our hemophilia center in Pittsburgh. Since the 2014 licensure we have switched 121 patients to extended half-life proteins. This included 85 with hemophilia A and 36 with hemophilia B. In our previously treated patients—that’s PTPs, people who had already been exposed to clotting factor before—we were able to use two doses per week. We tried this in children under a year of age—they were 8% of the group—those under eighteen years of age, and even those on immune tolerance. Among those in hemophilia B we switched patients who were previously treated because of the rarity of these new PUPs, but we found the same thing that we were able to get by with a dose every seven to ten days.
What is the impact on prophylaxis? What I really want to show you here is how we manage patients at our center. For prophylaxis we initiate it at their first bleed and do it once weekly. You ask yourself, “If the half-life is only 1.5-fold increase, how can you really do that?” Remember, we showed you that area under the curve. In our very young children usually below the ages of two, we are able to treat once weekly and avoid ports. This is such an improvement over what we had to do with recombinant products. It’s unbelievable and it works.
Breakthrough bleeds. If a patient starts having a breakthrough bleed, which often happens by the time they’re one, one and a half or two because of activity or severity of their disease, we just escalate it to twice weekly, and in almost every case the child had sufficient veins that we could have them come in twice a week.
What about in our inhibitor-prone children where we know the families have genotypes and members of the family who have had inhibitors? We started the drug once weekly before their first bleed considering some information about immune systems and their response to factor when they are already having bleeds. That has been extremely helpful in reducing the titer in a child who had a very high prone inhibitor compared with his maternal cousin who had to use recombinant factor VIII as his first drug. This child required a nine-month immune tolerance and had ports and hospitalizations, whereas the young man who started ITI with the same recombinant factor VIII Fc, he started before he had his first bleed and never needed ITI and is still on the drug. Now he’s using it twice a week and doing beautifully with no bleeds and no inhibitor.
For patients who are having a growth spurt, we cannot emphasize how critical it is to monitor their weight every three to six months, because many bleeds that occur in very young children occur because no one is monitoring their weight. We try to see young children every three to six months, and we try to make sure that all of our families have scales, because the dose is absolutely critically related to their weight.
What about ongoing bleeds? We discussed the treatment with the family and the child. If they want to play sports, we want them to play sports. If they have practice three times a week, then we’re looking at what do we need to do to get them through that practice so they don’t have a breakthrough bleed. How can we manipulate the dose? What are their troughs?
For the sports, the same thing. We assess their troughs. We assess dose frequency.
Here are some quotable quotes. Actually, I’ve heard them from a number of my colleagues—not just doubting families, but really from colleagues. Number one, the optimal trough is about 1%. Number two, extended half-life proteins are for severe patients only. Number three, extended half-life proteins are only for prophylaxis patients. Number four, extended half-life proteins should not be used in infants. Number five, extended half-life proteins are not for patients with inhibitors.
To these questions my answer is, “Not necessarily.” We have looked at a number of patients for whom the optimal trough can be 5%, like the patient Dr. Pipe showed us. We have had patients who are moderately severe who want to do sports or want to have an active life and have breakthrough bleeds unless they have a longer-acting protein. Number three, we have patients who are on demand, but when they have a bleed they like to have a protein that lasts longer than a day when they have a bad bleed, which is the kind they usually get. Number four, we have patients who are very young, and I’ve already given you a couple cases, we use it as the sole treatment in young children so we don’t have to use ports, so we don’t have to get inhibitors and so we can have families that have more normal lifestyles. Number five, they’re not for inhibitor patients. We have been able to show even if you develop an inhibitor, you can have tolerance occur in one month and you don’t have to have a port and go to the hospital umpteen times for an infection. This is life-changing therapy.
So, what is the evidence about the inhibitors? This is the mice data that I was telling you about. I really don’t want to belabor it, and I would also like to point out that while the mice data was in the recombinant factor VIII Fc protein, it’s been shown that the albumin Fc protein and the pegylated proteins also expand these T cells that make you more tolerant to the protein factor VIII or factor IX. We’re talking primarily here about factor VIII. What’s very exciting is the Fc portion of this molecule has been in many, many, many different drugs: Enbrel. Some of the biggest golfers in history use a drug which has Fc to make it last longer. It’s been used for over twenty years. Fc is used in many drugs. In hemophilia mice weekly factor VIII reduced the inhibitor significantly as compared with recombinant factor VIII. As I mentioned, we’ve already shown that it reduces not only the recurrence of an inhibitor; it reduces the titer and it makes the tolerance one month as opposed to nine months with no hospitalization and no ports.
When we manage our patients with extended half-life proteins, we have some questions for you. Is clinical or lab monitoring really necessary? Are pharmacokinetic studies needed? Do we have to do that on patients and bring them in for this stuff? What about breakthrough bleeds? Do we wait until they have a breakthrough and then change their dose? When should we increase or decrease the dose? I actually posed this question to Dr. Collins, who is a very brilliant pharmacokineticist, and it actually worked out that you only need two points in the pharmacokinetic study: one just after the dose is given and one just before the dose is given. So, in fact, you can bring your patient in one time and get both levels and know what their trough and their peak is.
In addition to that, you would want to know how well they’re doing clinically. Here is our case. This is one of my patients: an adolescent fifteen-year-old who had moderately severe hemophilia B who was very active in sports. He was on prophylaxis. He did basketball practice twice a week. He had games on the weekends. He was using recombinant factor IX and he did it one to two times per week, but he could never get up early enough in the morning, so he gave it at night. He had all kinds of bleeds. He had a hip bleed. He had recurrent ankle bleeds. Then he had a quick growth spurt that he forgot to tell us about, and we dosed him and he still was having bleeds.
So, what were the issues that should be raised when you want to switch somebody to recombinant factor IX? What should his starting dose be? Is a peak and trough necessary? These were the questions that we talked about with this family.
We began him on recombinant factor IX Fc of 75 units per kilogram once weekly. What we found with the 75-unit per kilogram dose was that he still had a breakthrough bleed, so we increased him after noting a trough of only 1% for him, a peak of a higher percent. We increased him to 100 units per kilogram once weekly. He went to 2% and he had very few, if any, breakthrough bleeds.
One of the things that I think we should come away with from this presentation is that a personalized approach is really the best approach. It’s what we do with our patients. It’s what should be done with every patient who has hemophilia. With sports, why not be feeling invincible? But you’ve got to have invincibility with responsibility, and I mean getting the trough and the peak and finding out if you have breakthrough bleeds and how often you’re going to be very active.
You need to take ownership with transition issues. When does the child begin to do self-infusion and order his factor and adjust and know when his practice and games are? One size clearly does not fit all. As I showed you with the Spotts data and many other patients that we were talking about, we need to understand not only their troughs and peaks, but we need to know how active they are. We need to know their growth spurts. We need to get frequent weights, especially as they’re going through the growth spurt and at least every three to six months we get those levels before we order and as they order factor.
Infants and children. One can start with a once-weekly dosing, because it’s clearly the simplest way to do this. It is easier on families. It avoids ports. It improves outcomes, because they don’t have bleeds. And when they do start having breakthrough bleeds it’s quite simple to increase it to twice a week. And in most children, by the time that happens, their veins are reasonable enough and large enough that they can then go to twice-weekly dosing.
One needs to have realistic expectations. We need to assess compliance in arthropathy. We’ve had several patients who said they really didn’t like the extended half-life protein, but they were skipping doses. If you want it to work, you need to make it work in a way that it only can, which is it lasts up to four to five days as a recombinant factor VIII Fc, and lasts seven to fourteen days as a recombinant factor IX Fc.
Also, if you have chronic arthropathy, it may be that you have a worse outcome in terms of pain, joint disability and you may need more frequent dosing.
Compliance. You really need to see how this works for you. Not everyone will respond. Most people do, but if you don’t, we need to look at your particular situation. If you find these drugs don’t work for you, we need to consider some of the more novel therapeutics, which I know Dr. Pipe and I have both done and have been absolutely dazzled. These were in clinical trials. So, don’t give up. And then of course chronic arthropathy may not improve if you already have it. Whether it will prevent it in the future is not known. That will require a prospective study.
We are very, very excited about the potential tolerogenicity of this recombinant factor VIII Fc. We have been talking to a number of centers to make sure they’re aware that we will be starting a phase II single-arm trial looking at previously untreated patients using Eloctate, which is recombinant factor VIII Fc, 50 units per kilogram just once a week. We’re going to be looking for the development of inhibitors. We’re not using ports. We have been able to perfect sample draws to less than 1 to 2 CCs to get all the data we need so that they’re not poked more than the time they’re poked to get the factor infused. And we’re going to be using a single IRB so that each site doesn’t have to do 99 times the same work that we’ve already done in our center.
Thank you.
KELLEY POLLARD: All right. Ladies and gentlemen, to ask a question via the web presentation, select the Chat Pod located in the lower left corner of your screen, then type and send your question. If you would like to ask a question live via your phone, please press star 1 on your telephone keypad. I will announce each caller prior to bringing you into the conference. Please remember if you have your phone on mute, take it off mute when you are selected to ask your question. Once again, to ask a question via the web presentation, select the Chat Pod located in the lower left corner of your screen, then type and send your question. To ask a question live, please press star 1 on your telephone keypad. All right. It looks like we’ve got a couple of questions that have come in. The first one reads, “Are either of you seeing improved adherence rates at your centers in patients on extended half-life products?”
DR. STEVEN PIPE: I would say yes, but maybe not in the way you would normally think. What I’m finding is this has opened up a whole new world of convenience for families. Because of the longer half-life, you have a little bit more flexibility on the timing of the next infusion. For instance, with the shorter-acting half-life products, the patient may have to strictly adhere to every 48 hours and they don’t really have an option to not give it in the morning and give it later in the day. With the longer-acting products I’m finding that the patients and families have a lot more freedom to flex the timing on their infusions. One thing that was really notable, we have a lot of busy dual professional families, sometimes multiple children. Those weekday infusions were particularly challenging and time consuming. With the twice-weekly-dosing pattern they were able to do one dosing on the weekends, like on a Sunday, and then the second dose would be done Wednesday afternoon or evening. What it did is it completely removed the hustle and bustle and pressure of trying to do infusions during weekdays early in the morning before the kids go to school or the parents go to work. So, from that standpoint, absolutely, this has been a significant improvement in adherence.
DR. MARGARET RAGNI: In adults I would have to say people who would not do prophylaxis because they refused to infuse three times a week, which is over the half the adults who previously used that sort of dosing, many have come to us and said, “I would be willing to do a twice-weekly dosing,” very much on the schedule Dr. Pipe was talking about. They pick the two days. They pick the time. And it really does make a very huge difference in willingness. I don’t know if the word would really be compliance, but in willingness to adopt the regimen that is required for those products. So, it’s been very exciting. Many more patients on prophylaxis should hopefully equate into better joint outcomes.
KELLEY POLLARD: And our next question is, “Why are the INHIBIT and HIRE studies being conducted with recombinant factor VIII Fc fusion protein and do not include other extended half-life products?”
DR. MARGARET RAGNI: That’s a very, very good question. This was the first protein that was approved by the FDA. In addition, it was the first one that we tried to get some preliminary data on, which is critical to having studies approved. One needs preliminary data, and the mice data with recombinant factor VIII Fc was much more extensive than any of the other products. However, there is no reason why it might not be the case that any other of the extended half-life proteins may do the same. But when one runs a clinical trial, one wants to try to reduce the amount of variability so that one can make sense of the clinical outcomes that one is looking at. By no means do we mean to say that the recombinant factor VIII Fc is the only extended half-life protein that may reduce inhibitors and shorten immune tolerance. That was the first drug approved by the FDA, and that was the first one we derived preliminary data on and are setting up a clinical trial around. It does not mean it’s the only one. In fact, I hope all of them do this.
KELLEY POLLARD: The next question is, “Can a rapid growth spurt in height impact successful prophy and no increases in weight?”
DR. STEVEN PIPE: That has to do a little bit with some detailed pharmacokinetics and some things that we call volume distribution, etcetera. I would say it depends. There could be height spurts that really don’t impact the pharmacokinetics at all, and then in other cases it may. I think it just begs the point that we should be seeing patients at least frequently enough so that we can keep tabs and we can identify when somebody is showing some evidence. So, maybe they’re not having the same efficacy anymore, they’re having a little bit more breakthrough bleeding and we can get trough levels at follow-up visits and have some assessment of how they’re doing in that regard.
DR. MARGARET RAGNI: Dr. Pipe, you’re absolutely right. That actually underscores how critical it is to keep up with your clinic visits and seeing your physician several times a year. I think it is absolutely critical, because we ask, “Have you had a bleed? What’s going on? How is your life? How are things going?” And by asking those questions, we immediately start to think about what might be changed or whether or not we need to get another trough level.
KELLEY POLLARD: How willing are patients to start on the extended half-life product? Is there a lot of fear?
DR. MARGARET RAGNI: What we do, as we do with every new product we’ve had since all the new products started in our long timeline of new products, is we really believe in is patient choice. In order to make an intelligent choice, one needs to have a good, intelligent set of data and information to choose from. What we do is we inform our patients at every clinic visit about what new clotting factors or proteins are available. We make clear what they might do for them. We make clear how we think they’re doing now and how a particular product might help them. We have no guarantees, but we show data. We talk about what happened in the clinical trials. We have amassed a lot of experience now in the last two-and-a-half years as the products became approved. We’re very active in clinical trials so that when someone is failing any product, if there is a novel protein in clinical trials, we want our patients to have that opportunity. Again, it’s patient choice. We talk with parents. We talk with children, especially our inhibitor patients who have such a hard time once they are refractory to intolerance, what’s the next step. I think some of these novel therapeutics have an incredible potential to change such a poor outcome as what happens with inhibitor patients.
KELLEY POLLARD: Are payers accepting extended half-life products? Are there significant issues on the cost?
DR. STEVEN PIPE: This is an evolving issue. I would say that it’s very payer dependent. In many cases we’ve been required to provide additional justification why an extended half-life is needed in a particular patient. I would say we’ve been able to provide that justification, it was accepted and the product was approved. In a few cases we had some families that chose not to switch at a particular time, because the out-of-pocket costs were too high. As different approvals were achieved with the regulatory agencies, those out-of-pocket costs became reduced and it became easier for them to switch. So, we do know that there is a first wave of payers who are issuing guidance and guidelines that the extended half-life products are not on their preferred drug list, that patients can get access to them, but you have to jump through some additional hoops. That’s probably just the reality of the cost premium of these products over the standard recombinants. I think it’s a reality of our health system. I think it’s going to continue to be this way going forward. As Dr. Ragni was showing at the end there, as long as we continue to do this research and we show the benefits of these molecules, and particularly the benefits on long-term outcomes, we won’t have any difficulty in justifying their use.
DR. MARGARET RAGNI: My experience has been that anyone who has wanted to be on those proteins has been able to go on them. We have a 340B program at my center, which I think makes things much easier. The only single problem we did face was a young man who wanted to play soccer nearly every day of the week at camp, and he did have some breakthrough bleeds despite being on an extended half-life Fc, so he just took somewhat higher doses. We have every-three-month conference calls with the insurance company. Other than that, we’re doing fine.
KELLEY POLLARD: Can you talk about mild or moderate patients and extended half-life products? Are you putting them in prophylaxis?
DR. MARGARET RAGNI: The purpose of prophylaxis is to prevent spontaneous bleeding by maintaining a level above 1%. Almost all of the mild and moderate patients do not have spontaneous bleeding. We do have an occasional moderate who does. But the bottom line is, especially for the moderate patients, if they’re very active and have frequent bleeds, we will talk with them about whether or not they would like to try the protein. Most of our milds tell us they don’t need it, and they’re absolutely right. As best I can tell, they’ve had one bleed in the last two years. I don’t think they need the protein. We also have some moderates who have frequent bleeding. If you tell them that once-a-week treatment is an option, they may consider it. But I would have to say very few of our moderates and none of our milds are on prophylaxis, but we let them know about these proteins. If they want to use it for their bad bleeds, as I mentioned before, the protein lasts for several days so that treatment may be sufficient.
KELLEY POLLARD: Thank you very much. That was the last question. I would like to thank you both. Ladies and Gentlemen, your feedback is critical to us, not only in evaluating this presentation, but in the planning of future webinars. Please complete this five-minute survey appearing on your screen now by clicking on the link. I’d like to thank you all for attending. And this concludes our program.
[END OF WEBINAR]