Read the latest press release from the All Copays Count Coalition
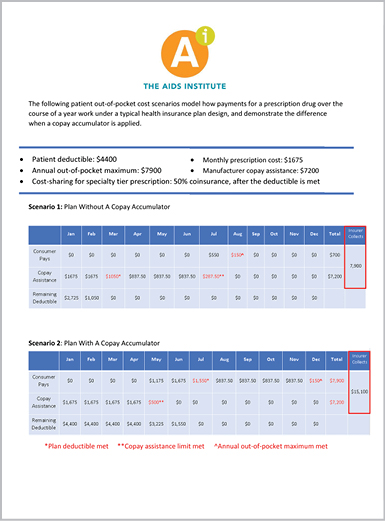
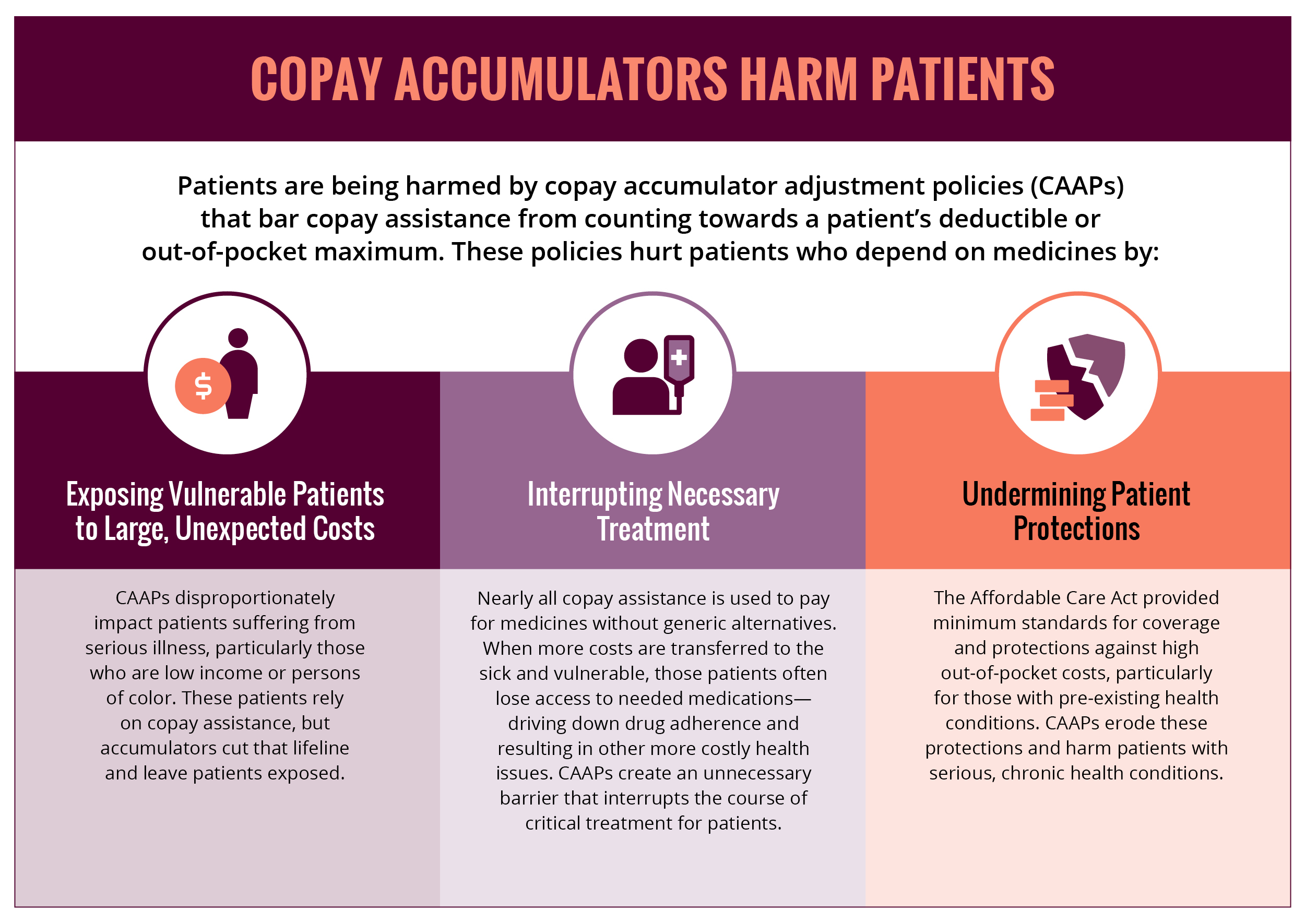
Millions of patients who depend on financial assistance to afford their medications are now being told that the money must come out of their own pocket before they can get their medications. Health plan policies called copay accumulator adjustments no longer count financial assistance toward the patient’s annual deductibles or their out-of-pocket maximum. In addition, a loophole in the Affordable Care Act allows many employer-sponsored health plans to deem certain critical and life-saving prescription drugs as “non-essential,” which significantly increases out-of-pocket costs for patients.
Together, these practices disproportionately target the most financially vulnerable patients with serious chronic health conditions, creating an affordability crisis and essentially undermining pre-existing condition protections.
National Bleeding Disorders Foundation, The AIDS Institute, and many patient communities are concerned about this issue—learn more about the All Copays Count Coalition.
 |
Policymakers Must Act to Protect Patients
We urge the Centers for Medicare and Medicaid Services to address these practices in the next Notice of Benefits and Payment Parameters (NBPP) by reversing the previous rulemaking that resulted in more patients being impacted by this harmful policy.

We also urge members of Congress to sign onto the
Help Ensure Lower Patient Copays Act (HELP Copays Act)
a two-part solution that requires health plans to count the value of copay assistance toward patient cost-sharing requirements and closes the essential health benefits (EHB) loophole to ensure specialty drugs are covered by health plans. Learn more about this legislation.
Watch videos to learn more about copay accumulators and how copay accumulator programs impact patients |
 |